An Afrobarometer survey found South Africans are deeply suspicious of Covid-19 vaccines, with nearly half of participants preferring prayer to the jab.
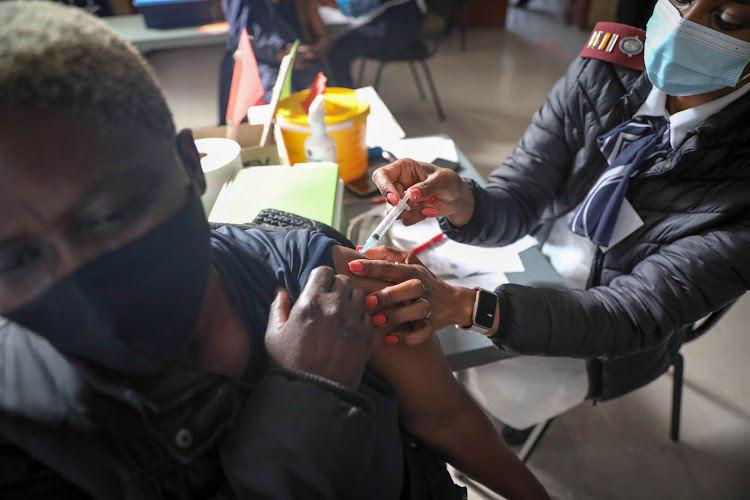
After a slow start that left South Africans both anxious and irate, our Covid-19 vaccine rollout has gained momentum in the past two months. With vaccine administration now up to over 150,000 doses per day, we are finally getting shots into South African arms.
But the greatest challenge facing the vaccine rollout is still to come. Vaccine hesitancy is a growing problem. Last week’s Afrobarometer survey findings show that South Africans are deeply suspicious of Covid-19 vaccines, with nearly half of survey participants reckoning on prayer rather than the jab to protect them from the ravages of this highly contagious virus.
Almost every country with an advanced vaccine rollout programme has experienced the flattening of an initially enthusiastic vaccine take-up curve. After an initial surge in vaccination numbers, rollout programmes tend to hit a ceiling, plateauing even though there are vaccines available and healthcare workers to administer them.
The US took just over two months to administer 58-million vaccines — equivalent to SA’s population — and by the end of April, just over four months into their rollout, 144-million people (44% of the population) had received at least one dose of a Covid-19 vaccine and over 100-million (31%) were fully vaccinated, at a rate often exceeding 1.5-million doses a day.
But since then the US rollout has gone cold. In the past month the average number of daily doses administered has been about 270,000, just a fifth of the rate initially achieved. Similar plateaus have occurred in the UK, Germany, the Netherlands and Canada.
The reason for this is the resistance of eligible individuals to receiving a vaccine, termed “vaccine hesitancy” by epidemiologists. The “5C model” has been developed by researchers to explain why it occurs. A lack of confidence in the safety and effectiveness of vaccines, coupled with complacency due to a perception that the risk of illness is low and vaccination is not necessary, are common reasons.
Constraints, including structural or psychological barriers like the inconvenience of being vaccinated and the fear of injections, are also prevalent. The vaccine hesitant also tend to calculate that their risk from vaccination outweighs the risk of infection and disease. Finally there is the absence of feeling a sense of collective responsibility (an individual’s willingness to protect others in the community through their own vaccination).
South Africans have already exhibited high rates of vaccine hesitancy, with a much slower rate of turnout being seen than was initially anticipated. The Afrobarometer findings showed that more than 54% of South Africans consider themselves unlikely to try to get vaccinated against Covid-19. Just 28% of respondents said they trust the government to ensure vaccines are safe.
The study suggests that the determinants of vaccine hesitancy — especially a lack of confidence and high complacency, and therefore an unfavourable risk calculation — are already at play. Many of these concerns are exacerbated by misinformation and alarmist anecdotes about vaccine side-effects circulated on social media.
We can’t wish every component of vaccine hesitancy away, but we can and should focus on minimising structural constraints to vaccination — and ensuring that the jabs that are administered are effective.
One of the most important of these constraints is the inconvenience faced by people living in rural areas in accessing vaccine sites, since they often incur high transport costs to reach clinics. While registrations for vaccines among people in rural areas are relatively high, it remains to be seen whether logistical challenges to rural vaccination will be surmountable and safe, accessible, and reliable sites are provided in remote areas.
Another key component is safety and efficacy, which influence confidence. Once Pfizer vaccines arrive in Johannesburg from overseas they are transferred to provincial distribution centres in thermal shipping boxes designed to keep the vaccines at the required —70°C using dry ice. It is critical that the dry ice is replaced every five days — something that can go wrong as a result of dry ice supply issues or, more commonly, when someone forgets to do maintenance.
After the vaccines are transported to the vaccination sites, the vaccines are transferred to an ordinary fridge, in which they can be stored for up to five days. But if the cold chain is broken at any point from arrival to administration the vaccines become ineffective.
The good news is that SA engineers and scientists are no strangers to solving complex problems. For example, a locally-hatched mobile cooling solution has been developed for the transportation and storage of vaccines that eliminates reliance on dry ice. Cryo-Vacc, as it is called, replaces the rudimentary dry-ice cooler-box system and relies on liquid nitrogen and long-life batteries, with a sophisticated and instant remote temperature monitoring system. Cryo-Vacc has longer storage periods, is unaffected by load-shedding, and minimises the risk of human error.
The device records any break in the cold chain through its monitoring system, which is publicly accessible through a mobile app. This means every patient can request the lot number of the vaccine they received, and use it to find out whether their vaccine was correctly transported and stored. This increases confidence, a key determinant of vaccine hesitancy.
While cold chain management is just one — though very crucial — part of ensuring a safe and effective rollout, it is clear that the talent and ingenuity exists in SA to ensure that we do everything we can to stave off vaccine hesitancy and inspire public confidence in the process. Government, if it is prudent, will ensure that it relies on this expertise as much as possible.
